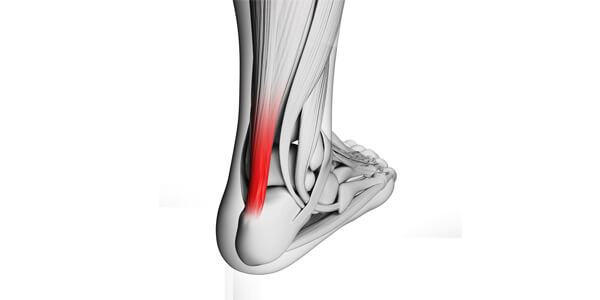
Ryan M, Wong A, Taunton J. Favorable outcomes after sonographically guided intratendinous injection of hyperosmolar dextrose for chronic insertional and midportion achilles tendinosis. Am J Roentgenol. 2010 Apr;194(4):1047-53.
Dr. Reeves’ Notes: This study involved patients with chronic tendon symptoms and all had objective evidence of Achilles degeneration by ultrasound at onset of the study. 108 tendons were treated in 99 patients. A median of 5 injections (1-13) were given, with ultrasound findings obtained at study onset and at plateau or symptom elimination point of 5-73 (mean 28) weeks. Treatment method involved injection inside the tendon with ultrasound monitor into areas of degeneration (hypoechogenicity or tear) with 0.5 ml or less dextrose 25% in 1-3 spots at each treatment. All patients were referred from sports medicine docs and had failed previous treatment. A follow-up contact attempt was made for all patients at 12 months following the last treatment for the last patient in the series. Follow ups ranged from 12 to 48 with a mean of 28 months. Although only 71% of patients could be reached for follow-up, notable is that improvement in pain with everyday living improved further. (From 57% at a mean of 28 weeks to 81% at a mean of 28 months.) Note that ultrasound changes at a mean of 28 weeks were more impressive in the mid Achilles tendinois group with significant reductions in size of hypoechoic regions, intratendinous tears and neovascularization. Note also that the symptomatic resolution in pain occurred despite neovessels still present in 60/108 cases (56%) at the mild to moderate level at the mean 28 week ultrasound follow up.
Click for a PDF copy of this study on Achilles tendinopathy.
AN ABSTRACT IS AVAILABLE BELOW.
OBJECTIVE
The objective of our study was to report on changes in the short-term sonographic appearance and 2-year follow-up for pain outcomes in a large patient population with chronic Achilles tendinosis who underwent sonographically guided dextrose injections.
SUBJECTS AND METHODS
One hundred eight tendons (86 midportion and 22 insertional) from 99 patients experiencing pain for greater than 6 months at either the Achilles tendon insertion or midportion were included in the study. Gray-scale (5–12 and 7–15 MHz) and color Doppler sonography examinations preceded the injection procedure using a 27-gauge needle administering a net 25% dextrose–lidocaine solution intratendinously. Structural features of each tendon and presence of neovascularity were noted. Visual analog scale (VAS) items were recorded at baseline, posttest, and 28.6 months follow-up.
RESULTS
A median of five (range, 1–13) injection consultations were needed for each patient, spaced 5.6 ± 3.1 (SD) weeks apart. There was a significant improvement in pain scores for both midportion (rest: 34.1 ± 27.7–3.3 ± 7.4, activities of daily living (ADL): 50.2 ± 25.6–9.5 ± 16.2, and sport: 70.7 ± 23.3–16.7 ± 22.0) and insertional (rest: 33.0 ± 26.5–2.7 ± 6.0, ADL: 51.3 ± 25.4–10.0 ± 16.3, and sport: 69.6 ± 24.5–17.7 ± 29.1) patients from baseline to follow-up for all VAS items. There were reductions in the size and severity of hypoechoic regions and intratendinous tears and improvements in neovascularity.
CONCLUSION
Dextrose injections appear to present a low-cost and safe treatment alternative with good long-term evidence for reducing pain from pathology at either the insertion or midportion of the Achilles tendon.
Robert J. de Vos, MD; et al., Platelet-Rich Plasma Injection for Chronic Achilles Tendinopathy, JAMA. 2010;303(2):144-149. doi: 10.1001/jama.2009.1986
This study was moderate in size with 27 in the PRP group and 27 in the saline group and good followup to data analysis point occurred without data loss. The VISA-A was used as the primary clinical measure. The VISA-A score is a measure specifically of Achilles pain and function. The authors, (despite decades of research showing that injection is not a placebo intervention), describe subcutaneous injection of marcaine 0.5%, followed by intratendinous needling with saline in 5 separate aliquots, as a “placebo” intervention. The authors unfortunately missed an excellent opportunity to have an exercise control by not assigning a group of patients to exercise only. They also did not have a group with injection only. (See Yelland et al 2009 study on Achilles Tendinopathy for a better study design)
A review of the two groups characteristics before treatment revealed that the duration of symptoms was 10 weeks longer in the PRP group (36 vs 26), and that only 1/4 as many in the PRP group were able to play sport unchanged (9% versus 37%). Despite that, 10% more in the PRP group were playing their desired sport at the 6 month period. (78% versus 67%).
So, essentially, this study was a treatment comparison study, not a placebo study, and had potentially dissimilar groups. Nevertheless, this study does make a statement about the potential limitations of any one injectant over another in conditions unless the pathology is more fully understood. In this case, in those doing eccentric lengthening exercises, a single injection session with PRP appears to be no more efficacious than saline injection.
Brian Shiple commented on the major problems with this study in a very useful way. A few thoughts of his are offered here:
Comment #1: “In our experience, the two pathologies that are the most recalcitrant to treatment with PRP are chondromalacia patellae and Achilles tendinopathy. In over two years of doing PRP, we have NEVER had a patient with chronic Achilles tendinopathy heal after only one treatment. It typically takes 3–4 treatments and 6 months or more, combined with eccentric exercise. And even with that, the success rate is much lower than with epicondylosis, patellar tendon, etc.”
Note that basic research means that you use a treatment approach that you expect to be effective. What Dr. Shiple is saying is that this study used completely in appropriate dosing to try to prove something. It is like studying defibrillation at 1/10th normal voltage versus pounding on the chest and finding that neither one in the patient with a shockable rhythm cardiac arrest.
Comment #2: “Did these patients have paratenon disease either on exam or by U/S? If they did and this was not treated, they don’t get better in our experience. Some authors have described the achilles tendon disease as acutally 4 separate and distinctly different disease states: 1) mid portion tendinosis; 2) mid portion paratenon tendinitis/osis; 3) mid portion acute complete tear; 4) mid portion partial tears with coexisting tendinosis. And then there is the insertional tendon issues which behave differently than the mid portion ones. Plus you can have a combination of these conditions above. So if they had 60% of these cases with tendinosis with paratenon disease and the paratenon was not treated you would have 60% doing equally poorly.”
Achilles studies need to be more precise about what they are actually studying as different conditions respond differently and this affects outcomes and group comparisons a great deal.
The complete study for Platelet-Rich Plasma Injection Versus Saline injection, including abstract, is available here.
Vos RJ, Weir AW, vanSchie HTM, Bierma-Zeinstra SMA, Verhaar JAN, Weinans H, Tol J. Platelet-Rich Plasma Injection for Chronic Achilles Tendinopathy: A randomized controlled trial. JAMA 2010 303(2):144-148.
An abstract of Platelet-Rich Plasma Injection for Chronic Achilles Tendinopathy is available here, with a copy of the content below.
CONTEXT:
Tendon disorders comprise 30% to 50% of all activity-related injuries; chronic degenerative tendon disorders (tendinopathy) occur frequently and are difficult to treat. Tendon regeneration might be improved by injecting platelet-rich plasma (PRP), an increasingly used treatment for releasing growth factors into the degenerative tendon.
OBJECTIVE:
To examine whether a PRP injection would improve outcome in chronic midportion Achilles tendinopathy.
DESIGN, SETTING, AND PATIENTS: A stratified, block-randomized, double-blind, placebo-controlled trial at a single center (The Hague Medical Center, Leidschendam, the Netherlands) of 54 randomized patients aged 18 to 70 years with chronic tendinopathy 2 to 7 cm above the Achilles tendon insertion. The trial was conducted between August 28, 2008, and January 29, 2009, with follow-up until July 16, 2009.
INTERVENTION:
Eccentric exercises (usual care) with either a PRP injection (PRP group) or saline injection (placebo group). Randomization was stratified by activity level.
MAIN OUTCOME MEASURES:
The validated Victorian Institute of Sports Assessment-Achilles (VISA-A) questionnaire, which evaluated pain score and activity level, was completed at baseline and 6, 12, and 24 weeks. The VISA-A score ranged from 0 to 100, with higher scores corresponding with less pain and increased activity. Treatment group effects were evaluated using general linear models on the basis of intention-to-treat. RESULTS: After randomization into the PRP group (n = 27) or placebo group (n = 27), there was complete follow-up of all patients. The mean VISA-A score improved significantly after 24 weeks in the PRP group by 21.7 points (95% confidence interval [CI], 13.0-30.5) and in the placebo group by 20.5 points (95% CI, 11.6-29.4). The increase was not significantly different between both groups (adjusted between-group difference from baseline to 24 weeks, –0.9; 95% CI, –12.4 to 10.6). This CI did not include the predefined relevant difference of 12 points in favor of PRP treatment.
CONCLUSION:
Among patients with chronic Achilles tendinopathy who were treated with eccentric exercises, a PRP injection compared with a saline injection did not result in greater improvement in pain and activity. Trial Registration Identifier: NCT00761423 (clinicaltrials.gov)
Yelland MJ, Sweeting KR, Lyftogt JA, Ng SK, Scuffham PA, Evans KA. Prolotherapy injections and eccentric loading exercises for painful Achilles tendinosis: a randomised trial [epub ahead of print] Br J Sports Med (England), Jun 22 2009, pages pending.
This study also used the VISA-A. This study was a superior design to Vos et al because there was an exercise only group as the control. In addition there was an injection only group that did not exercise. It is important to note that eccentric lengthening exercises (ELE), the exercise approach used, is not a placebo intervention, and is commonly used in the sports medicine community. ELE is particularly effective in mid portion Achilles tendinopathy which these patients had. The injection group was not an intratendinous injection but rather involved simple subcutaneous injection of dextrose without radiographic guidance.
Injections were repeated weekly in the injection group. Thus this study was a treatment comparison study of usual treatment (ELE) versus injection treatment versus combined exercise and injection. It is of interest that reduction of stiffness and limitation of activity was faster with dextrose injection, and that combining both eccentric loading and dextrose injection combined was significantly better than eccentric activity alone. A larger study will be of much interest if funding is available.
An abstract of dextrose prolotherapy versus eccentric loading exercises is available here, with a copy of the content below.
OBJECTIVE:
To compare the effectiveness and cost-effectiveness of eccentric loading exercises (ELE) with prolotherapy injections used singly and in combination for painful Achilles tendinosis.
DESIGN:
A single-blinded randomised clinical trial. The primary outcome measure was the VISA-A questionnaire with a minimum clinically important change (MCIC) of 20 points on a 100 point scale.
SETTING:
Five Australian private primary care centres.
PARTICIPANTS:
43 patients with painful mid-portion Achilles tendinosis commenced and 40 completed the treatment protocols.
INTERVENTIONS:
Participants were randomised to a 12 week program of ELE (n=15), or prolotherapy injections of hypertonic glucose with lignocaine alongside the affected tendon (n=14) or combined treatment (n=14). Main outcome measurements: VISA-A, pain, stiffness and limitation of activity scores and treatment costs were assessed prospectively over 12 months.
RESULTS:
At 12 months, the proportions of participants achieving the MCIC for VISA-A scores were 73% for ELE, 79% for prolotherapy and 86% for combined treatment. Mean (95% CI) increases in VISA-A scores at 12 months were 23.7 (15.6 to 31.9) for ELE, 27.5 (12.8 to 42.2) for prolotherapy and 41.1 (29.3 to 52.9) for combined treatment. At 6 weeks and 12 months, these increases were significantly less for ELE than for combined treatment. Compared with ELE, reductions in stiffness and limitation of activity occurred earlier with prolotherapy and reductions in pain, stiffness and limitation of activity occurred earlier with combined treatment. Combined treatment had the lowest incremental cost per additional responder (AU$1539) compared with ELE.
CONCLUSIONS:
For Achilles tendinosis, prolotherapy and particularly ELE combined with prolotherapy give more rapid improvements in symptoms than ELE alone but long term VISA-A scores are similar.
Orchard J; Massey A; Brown R; Cardon-Dunbar A; Hofmann J. Successful management of tendinopathy with injections of the MMP-inhibitor aprotinin. Clin Orthop Relat Res (United States), Jul 2008, 466(7) p1625-32
Injection of Solutions that block breakdown of tissue may also help healing. Metalloproteinase (Collagenase is an example) breaks down issue and an inhibitor of metalloprotinease has been found to help some cases of tendon damage.
An abstract of Achilles and Patellar Tendon: Aprotinin injection is available here, with a copy of the content below.
Aprotinin is a broad spectrum proteinase inhibitor (including matrix metalloproteinase [MMP] inhibitor) used for treating patellar and Achilles tendinopathies. One previous randomized control trial demonstrated aprotinin injections superior to both corticosteroid and saline injections in patellar tendinopathy (Level II), whereas results reported for aprotinin treatment in Achilles tendinopathy have been mixed. We performed a case review and follow-up questionnaire for 430 consecutive patients with tendinopathy treated by 997 aprotinin injections (30,000 KIU). A response rate of 72% was achieved with a minimum followup of 3 months (average, 12.2 months; range, 3-54 months). Seventy-six percent of patients had improved, 22% of patients reported no change, and 2% were worse. Sixty-four percent of patients thought aprotinin injections were helpful, while 36% believed they had neither a positive nor negative effect. Mid-Achilles tendinopathy patients (84% improvement) were more successfully treated than patellar tendinopathy patients (69% improvement). Despite stronger published evidence of benefit in patellar tendinopathy, clinical outcomes appeared better with aprotinin use in Achilles tendinopathies.
LEVEL OF EVIDENCE:
Level IV, case series.
Achilles Tendonopathy DEX: Maxwell et al 2007 Dextrose 25% injection in chronic Achilles strain resulted in ultrasound documented healing. Maxwell NJ, Ryan MB, Taunton JE, Gillies JH, Wong AD. Sonographically guided intratendinous injection of hyperosmolar dextrose to treat chronic tendinosis of the Achilles tendon: a pilot study. JR Am J Roentgenol. 2007 Oct;189(4):W215-20.
In 2007 the Department of Radiology in Vancouver, BC, Canada published study in which 25% dextrose was injected in chronic Achilles strain. Their results showed pain with sport decreased 78% and by X-Ray the tendons became more healthy, as seen by less holes in the tendon, and better organization of tendon fibers. There is some evidence that abnormal blood vessels (neovessels) develop in chronic strain and these themselves can be sources of pain. The X-Ray findings also showed that these blood vessels shrank. maxwellnj@upmc.edu
Helpful information from the primary author indicates that 36 patients began the study, 1 was not completed due to obvious high grade partial tear noticeable during ultrasound observation of injection, 3 were not included as they had obvious calcific tendinopathy that correlated with their lack of improvement after 4 treatments., and 2 were non contactable. This raises the question about calcific tendinopathy and how to address it differently or to screen it out so that an intention to treat approach to data gathering can be used. The phone interviews were performed a mean of 12 months post injection (4.5 -28 months). If the patient was making progressive improvement in symptoms the injection were continued until complete symptom elimination or until the patient was happy with the pain level or until plateau. It is important to note that abnormal areas in the tendon and intrasubstance partial tears were targeted rather than neovessels. It is also important to note that neovascularity decreased in many of these patients even without directly targeting the neovessels, but neovascularity was present in 88% of the tendons.
An abstract is available below.
OBJECTIVE:
Chronic tendinosis of the Achilles tendon is a common overuse injury that is difficult to manage. We report on a new injection treatment for this condition.
SUBJECTS AND METHODS:
Thirty-six consecutive patients (25 men, 11 women; mean age, 52.6 years) with symptoms for more than 3 months (mean, 28.6 months) underwent sonography-guided intratendinous injection of 25% hyperosmolar dextrose every 6 weeks until symptoms resolved or no improvement was shown. At baseline and before each injection, clinical assessment was performed using a visual analogue scale (VAS) for pain at rest (VAS1), pain during normal daily activity (VAS2), and pain during or after sporting or other physical activity (VAS3). Sonographic parameters including tendon thickness, echogenicity, and neovascularity were also recorded. Posttreatment clinical follow-up was performed via telephone interview.
RESULTS:
Thirty-three tendons in 32 patients were successfully treated. The mean number of treatment sessions was 4.0 (range, 2-11). There was a mean percentage reduction for VAS1 of 88.2% (p < 0.0001), for VAS2 of 84.0% (p < 0.0001), and for VAS3 of 78.1% (p < 0.0001). The mean tendon thickness decreased from 11.7 to 11.1 mm (p < 0.007). The number of tendons with anechoic clefts or foci was reduced by 78%. Echogenicity improved in six tendons (18%) but was unchanged in 27 tendons (82%). Neovascularity was unchanged in 11 tendons (33%) but decreased in 18 tendons (55%); no neovascularity was present before or after treatment in the four remaining tendons. Follow-up telephone interviews of the 30 available patients a mean of 12 months after treatment revealed that 20 patients were still asymptomatic, nine patients had only mild symptoms, and one patient had moderate symptoms.
CONCLUSION:
Intratendinous injections of hyperosmolar dextrose yielded a good clinical response–that is, a significant reduction in pain at rest and during tendon-loading activities–in patients with chronic tendinosis of the Achilles tendon
Alfredson H; Lorentzon R: Sclerosing polidocanol injections of small vessels to treat the chronic painful tendon.: Cardiovasc Hematol Agents Med Chem (Netherlands), Apr 2007, 5(2) p97-100
This is a 2 year followup report by Dr. Alfredson showing sonographic remodeling with a thinner tendon and more normal structure. By using ultrasound (US) + colour Doppler (CD), immunohistochemical analyses of tendon biopsies, and diagnostic injections of local anaesthesia, sensory nerves (Substance-P-SP and Calcitonin Gene Related Peptide-CGRP) were found inside and outside the vascular wall. In following clinical studies we have demonstrated good short-and mid-term clinical results using treatment with US+CD-guided sclerosing polidocanol injections, targeting the area with neovessels outside the tendon. Two-year follow ups have showed remaining good clinical results, and sonographically signs of remodelling with a significantly thinner tendon with a more normal structure. Whether the effects of polidocanol are mediated through destruction of neovessels, activity on nerves or a combination, is under evaluation.
Alfredson H; Ohberg L Sclerosing injections to areas of neo-vascularisation reduce pain in chronic Achilles tendinopathy: a double-blind randomised controlled trial. Knee Surg Sports Traumatol Arthrosc May 2005, 13(4) p338-44.
Injection of small amount of polidocanol were targeted using, ultrasound and color doppler guidance, to areas of abnormal small blood vessels found just outside the tendon on the anterior (deeper) side. The control group received anesthetic injection to the same areas. 5/10 patients in the polidocanol group responded to treatment within 2 treatments and the additional 5 responded to additional treatment. 0/10 of the anesthetic patients responded to 2 treatments, but this group then received polidocanol injection and 9/10 responded.
An abstract of Achilles Tendon Polidocanol is available here, with a copy of the content below.
Local injections of the sclerosing substance Polidocanol has been demonstrated to give good clinical results in a pilot study on patients with chronic Achilles tendinopathy. In this study, 20 consecutive patients (9 men and 11 women, mean age 50 years) with chronic painful mid-portion Achilles tendinopathy were randomised to injection treatment with either Polidocanol (5 mg/ml) (group A) or Lidocaine hydro-chloride (5 mg/ml) + Adrenaline (5 microg/ml) (group B). Both substances have a local anaesthetic effect, but Polidocanol also has a sclerosing effect. The patients and the treating physician were blinded to the substance injected.
The short-term effects were evaluated after a maximum of two treatments, 3-6 weeks apart. Before treatment, all patients had structural tendon changes and neo-vascularisation demonstrated with US and color doppler. Under US and color doppler-guidance, the injections targeted the area of neo-vascularisation just outside the ventral part of the tendon. For evaluation, the patients recorded the severity of Achilles tendon pain during tendon loading activity, before and after treatment, on a VAS. Patient’s satisfaction with treatment was also assessed. At follow-up (mean 3 months) after a maximum of two treatments, 5/10 patients in group A were satisfied with the treatment and had a significantly reduced level of tendon pain (p < 0.005). In group B, no patient was satisfied with treatment. In the pain-free tendons, but not in the painful tendons, neo-vascularisation was absent after treatment.
After completion of the study, treatment with Polidocanol injections (Cross-over in group B and additional treatments in group A) resulted in 10/10 and 9/10 satisfied patients in group A and B, respectively. In summary, injections with the sclerosing substance Polidocanol have the potential to reduce tendon pain during activity in patients with chronic painful mid-portion Achilles tendinopathy.